
Periodontitis ( Advanced Gum Disease ): Treatment and Symptoms

Gingivitis and periodontitis are two common dental conditions that affect the gums and supporting structures of the teeth.
Both conditions are characterized by gum disease and by inflammation of the gums crooked teeth, but they differ in terms of severity of gum disease and the extent of damage caused loose teeth by gum disease and gum inflammation.
Gingivitis is the milder form of gum disease and is usually reversible with proper treatment and good oral hygiene practices.
It occurs when plaque, a sticky film of bacteria, builds up on the teeth bleeding gums and along the gumline. The bacteria in plaque release toxins that irritate the teeth and gums below, leading to inflammation.
Common symptoms of gingivitis include redness, swelling, and bleeding of the teeth and gums below, especially during brushing or flossing. However, gingivitis does not involve any serious tooth loss or bone loss because of bone or connective tissue receding gums that support the teeth.
If left untreated, gingivitis can progress to periodontitis.
Periodontitis is a more advanced stage of the gum line, disease called gingivitis, characterized by the destruction of the gum line plaque and tartar line supporting structures of the teeth, including the gums, periodontal ligament, and alveolar bone.
As the periodontal disease progresses, the gum line and pockets deepen, allowing more bacteria to accumulate and cause further damage to gum disease. The immune system’s response to the infection can also contribute to the destruction of the gum line supporting tissues.
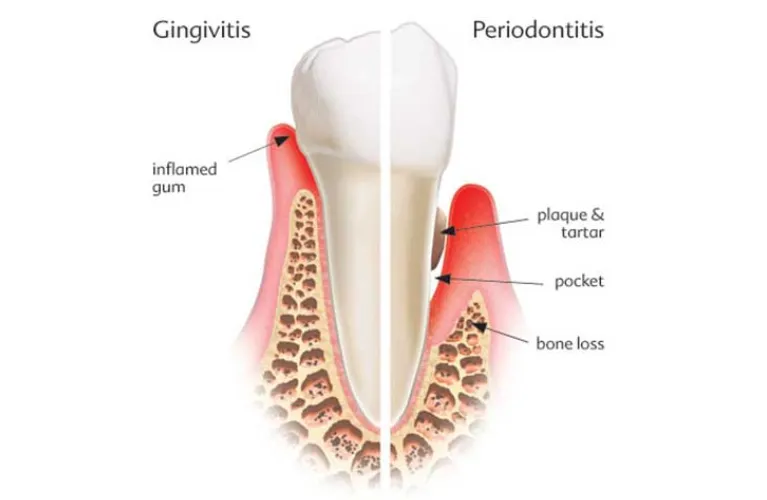
What are the symptoms of periodontitis?
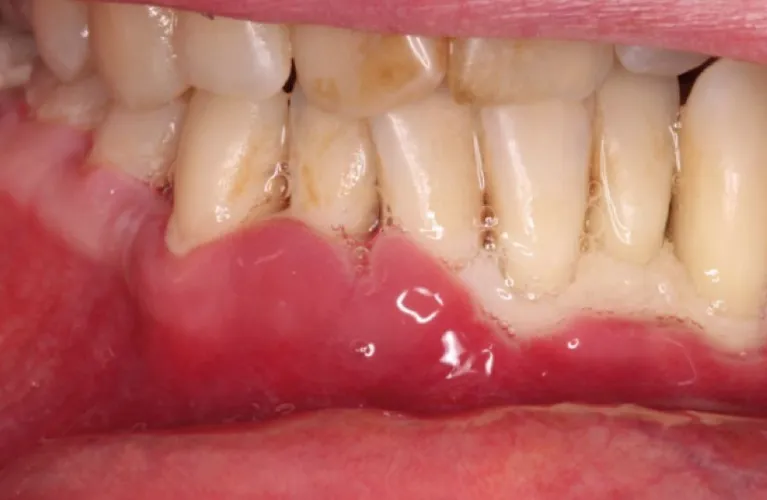
Healthy gums are firm to the touch and fit snugly around your teeth. In comparison, periodontitis has loose teeth and symptoms include:
- Reddish or purplish gums.
- Swollen gums.
- Gums that bleed easily.
- Tender bleeding gums.
- Bad breath.
- Pus (infection) around your gum line.
- Loose teeth.
- Tooth loss.
- Gum recession (when your gums pull away from your teeth).
- Pain when chewing.
- New gaps or spaces between your teeth.
- Changes in the way your teeth fit together.
What are the types of periodontitis?
Periodontitis is a group of inflammatory diseases that affect the tissues surrounding and supporting the teeth. There are several types of periodontitis, which can be categorized based on their characteristics and disease progression alone. Here are some common types of periodontitis:
Chronic periodontitis: This is the most common form of periodontitis. It progresses slowly and is characterized by inflammation of the gingiva (gums) and gradual loss of attachment between the teeth and supporting structures. It can lead to the formation of periodontal pockets and bone loss over time.

Aggressive periodontitis:
Aggressive periodontitis is characterized by rapid progression of attachment loss and bone destruction. It typically affects younger individuals and may involve a familial or genetic predisposition. Aggressive periodontitis can affect localized areas or the entire mouth.
Necrotizing periodontal diseases
This type of periodontitis is characterized by the death of gingival tissues (necrosis). Necrotizing periodontal diseases are often associated with systemic conditions such as HIV infection, malnutrition, or immunosuppression. They can cause severe pain, gum ulceration, and tissue destruction.

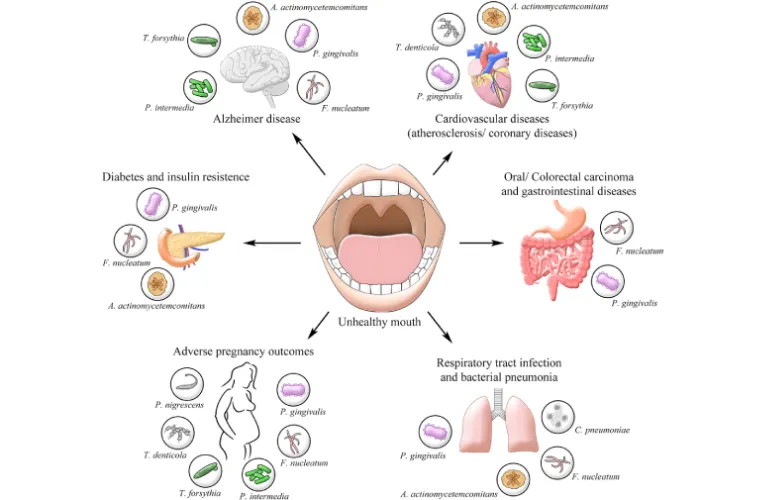
Periodontitis associated with systemic diseases
Certain systemic conditions, such as diabetes, heart disease, and respiratory diseases, can contribute to the development or progression of periodontitis. This type of periodontitis is referred to as periodontitis associated with systemic diseases.
Periodontitis as a manifestation of systemic diseases
Some systemic conditions can manifest in the form of periodontal destruction. For example, conditions like leukemia or genetic disorders can present with periodontitis as one of their symptoms.
It’s important to note that the classification of periodontitis may vary based on different classification systems and the terminology used by various dental health professionals.
How is periodontitis treated?
Nonsurgical periodontitis treatment
Nonsurgical options often work well for people with mild to moderate periodontitis. These treatments include:
Antibiotics: Your dentist may prescribe oral antibiotics to fight infection. Or they may place a topical antibiotic underneath your gums to target the affected area.
Scaling and root planning: Also known as deep dental cleaning, scaling and root planing are similar to routine cleaning. The difference between regular dental check ups scaling and root planing is that you’ll receive local anesthesia to numb your teeth and gums first.
Surgical periodontitis treatments
There are different types of surgical periodontal treatments, including:
Flap surgery:
In this procedure, the gums are lifted or folded back to expose the tooth roots and underlying bone. The dentist then removes bacteria and tartar from the deep pockets and may also perform bone reshaping or regeneration if necessary. Finally, the gums are repositioned and stitched back into place.
Bone grafting:
This procedure involves placing bone grafts or bone-like materials in areas where bone loss has occurred due to periodontal disease. The grafts stimulate new bone growth and aid in the regeneration of bone tissue.
Guided tissue regeneration (GTR):
GTR is performed in conjunction with flap surgery to encourage the growth of new bone and gum tissue. A barrier membrane is placed between the tooth roots and the gums, preventing gum tissue from invading the area while allowing bone cells to regenerate.
Soft tissue grafting:
This procedure is used to address gum recession caused by periodontal disease. A small piece of tissue is taken from the patient’s palate or another donor source and placed over the exposed tooth roots. This helps to cover the root surfaces and prevent further gum recession.
Prevention and home remedies
Home treatment is essential for the early stages of gum disease to control managing the bacterial plaque buildup of gum disease and the early stage of gum disease to control reducing the other risk factors of gum disease.
The American Dental Association (ADA) gives dental professionals the following advice:
- Brush the teeth for 2 minutes twice daily with a soft-bristle manual or electric toothbrush.
- Use fluoride toothpaste.
- Be sure to brush all surfaces.
- Replace the toothbrush every 3 to 4 months, or more often if the bristles are matted or frayed.
- Choose a brush with the ADA seal of acceptance.
Which toothpaste is best to use?
People should not share brushes, as harmful bacteria that can pass between individuals in this way.
A dentist can also advise on oral health conditions and other health conditions:
- dental floss or floss sticks
- interdental brushes
- antiseptic mouthwash
What are the best practices for healthy teeth and gums?
Other prevention tips include trusted Source:
- avoiding or quitting smoking
- limiting alcohol intake
- following a diet that contains plenty of whole foods and fresh fruits and vegetables
- visiting a dentist at least once a year
- working with a doctor to manage diabetes
- drinking plenty of water
Treatment
Treatment aims to clean out bacteria bacterial plaque from the tooth, bone, tooth, bone loss itself, the teeth properly, the pockets around the teeth lost bone, and prevent further destruction of bone and tissue.
Good oral hygiene
Good oral hygiene practices can help reduce the various risk factors of periodontitis.
Tips include trusted Source:
- brushing teeth at least twice a day
- flossing and using interdental brushes or soft picks once a day
- visiting a dentist at least once a year
- avoiding tobacco use
- limiting consumption of alcohol and foods with added sugars
- seeking dental or medical advice for dry mouth, changes in taste or smell, and other mouth problems
FAQ
How can you fix gingivitis?
Apply mouthwash to remove plaque. Ensure you brush and floss regularly using a special dental tool or brush for cleaning the interdental area. Get your teeth professionally cleaned every 3 years according to your dentist regularly your doctor’s recommendations.
How curable is gingivitis?
In contrast with periodontitis progresses other phases of gum disease, gingivitis can still be prevented with proper prevention and treatment. If you see any signs of gingivitis or other symptoms, then you may need immediate dental professional oral care. Untreated gout can progress severe periodontitis and lead to advanced periodontal disease too.
Can I get rid of gingivitis on my own?
You can eliminate bacterial plaque in gingivitis with natural home remedies such as oil extraction for killing bad bacteria or salted water wash for healing gingival wounds. Salted water rinses can also heal bleeding gums even after periodontal surgery for gingiva.
Is gingivitis a fungal infection?
Gingivitis are commonly known as gum disease. It is gum inflammation that occurs when bacteria build up inside your teeth.
What is the fastest way to cure gingivitis?
What is the most effective treatment for gingiva? You need to brush your teeth regularly two times. Use a soft toothbrush for squeezing your teeth properly. Give them floss twice daily. Plaque likes hiding between teeth so the brush bristle doesn’t get through. … Use fluoride mouthwash. … Please avoid dental appointments. “… Avoid sugary foods or beverages.
How can I treat gingivitis on my own?
It is actually possible to treat gingivitis severe gum disease on your own with a simple home remedy. Saltwater mouth rinses help with the healing of gums following a gum surgery.
What is the medicine for gingivitis?
Chlorhexidine is a dental anti-bacterial agent used for the treatment of gums and dental plaque. The drugs are available as mouthwash, or as gelatin infused chips placed into pocket after root planning.
Can gum gingivitis be cured?
Its cure is usually as soon as treatment begins to reduce symptoms of cardiovascular disease, gum disease, and heart disease itself. If your symptoms of gingivitis are visible in your mouth, make an appointment to the dentist. If heart and disease control is left in the hands of a dentist, it can become a serious gum disease again.
What are the 4 signs of periodontal disease?
Symptoms Bad breath or a bad breath or taste will never disappear. Red or swelling gum. Teeth and blood. Painfully chewed.
Can periodontitis be cured?
There’s nothing to be done with paranatomy. This includes poor oral hygiene and poor oral health as well as regular dental cleanings based good on oral health and good oral hygiene, on the recommended dental examination schedule by a dentist.
How do you know if you have periodontitis?
Periodontal disease has a number of symptoms including swelling of the teeth and gums, and puffiness. Dark red and dark purple teeth. The gum feels warm when touched.
What is the best periodontal treatment?
Developing good oral hygiene and planning. This deep cleaning technique has helped reduce increased risk of gum disease. Plaque and calculus are extracted from gum tissue through a hand scaling machine and/or ultrasonic equipment.
